Addiction is a public health crisis, and fear is beginning to give way to life-saving solutions.
The rapid national rise in heroin overdose deaths began in 2010. Many cite that year’s crackdown on prescription painkiller abuse as a cause, pushing users toward heroin as a prescription-free, readily available and cheaper alternative. Others blame a drug cartel push for greater trafficking throughout the U.S. that year, increasing supply and driving down prices. Still others point to a rise in heroin laced with fentanyl—a fast-acting narcotic analgesic and sedative—a far more potent version of the drug. Whatever the cause, the death toll is still ticking.
The National Institute on Drug Abuse cites 10,574 heroin overdose deaths in the U.S. in 2014—a six-fold increase from 2001—and 18,893 prescription opioid overdose deaths that year, more than tripling over the same time period. According to the CDC, heroin use was highest among males, 18-to-25-year-olds, non-Hispanic whites, those who make less than $20,000 annually and those residing in the Northeast—but in general, its use among all demographic subgroups is on the rise.
Peoria is not immune to these trends. Over the last five years, 57 people have died of heroin overdoses in Peoria County. In 2015 alone, 36 Peoria County deaths (plus an additional 13 from neighboring counties) were attributed to illicit drugs or prescription medication intoxication. By reducing a complex issue to sheer statistics, however, addiction loses its human face. On their own, the numbers ignore the full story: from the science of addiction to societal potholes on the road to recovery, and from the unspoken space between medical care and illegal activity to the financial burdens and emotional tolls of drug dependence. Instead, there is fear.
“People are so afraid of heroin in their communities that it makes [a solution] very difficult,” suggests Kathie Kane-Willis, cofounder and director of the Illinois Consortium on Drug Policy (ICDP), a research and policy institute housed at Roosevelt University in Chicago. “But the response needs to be more than fear.”
The Science of Addiction
The leap from abuse of prescription pain medications (such as hydrocodone, oxycodone, morphine and methadone) to heroin is not surprising—they belong to the same class of drugs. In fact, four out of five heroin users initiated their habit by misusing prescription opioids, according to a recent fact sheet released by the White House.
“All opioids are similar in that they attach to receptors that mediate pain, which are found in the nervous system, brain and elsewhere in the body,” explains Dr. Leon Yeh, Vice President and Chief Medical Officer of Emergency Services at OSF Healthcare System. More than 12 percent of the 571 overdose/abuse patients treated by the OSF Saint Francis Emergency Department last year were heroin-specific cases.
“When opioids are abused over time, the body’s own naturally occurring chemicals, such as endorphins, are reduced,” Dr. Yeh explains. Thus, when a person stops abusing opioid medications, the body is left with few natural opioids to act in the nervous system, which leads to withdrawal symptoms.
Both substance abuse and addiction are classified as diseases, Dr. Yeh adds, which should dispel the oft-perpetuated myth that drug addiction is somewhat voluntary—that people can stop using if they really want to. As such, medically based, primary care substance abuse treatment programs are the only proven road to full recovery from addiction—and to this end, Peoria’s options are vast.
The Illinois Institute for Addiction Recovery at Unity Point Health – Proctor, for one, offers both inpatient and outpatient services to adults and adolescents seeking recovery from addiction. In Pekin, the Gateway Alcohol & Drug Treatment Center offers outpatient rehab programs for adults and teens. “Addiction medicine has really come a long way,” suggests Executive Director Kerry Henry. “Those days of terrible withdrawal and painful detoxes are mediated now with the use of medication.” Other area treatment centers, like the Knolls Center for Change, Human Service Center and Teen Challenge, among others, offer a range of similar options for initial treatment.

But long-term recovery requires continued support, and in this space, the region’s options are more limited. For instance, the area has no Oxford Houses—the self-supporting, drug-free homes proven to help prevent relapse following addiction treatment—and until recently, there were no local sober living environments (SLEs)—the interim facilities that help recovering addicts bridge the gap between rehab and their future lives.
“We have great treatment centers… but research has shown that it’s so important for men and women who have the disease of addiction to stay in with people who are in recovery,” says Camilla Rabjohns. “They need to be with those people for a while to get their brain back in equilibrium.”
A Personal Mission
Tucked off a snow-laden drive in the woods between Glasford and Hanna City, Camilla and her son, Nick Rabjohns, stand in the warm basement of a rustic-looking cabin, looking out toward the woods. “In the summer, we have hummingbirds… There’s deer, raccoons and coyotes, though I’ve still only heard them—never seen them,” Nick says, between sips of coffee.
Observing nature can be healing—a way “to get out of your own self and think about others and meditate,” Camilla adds, pointing out the walking trails they started clearing last summer.
Mother and son offer a tour of the fully-furnished, four-bedroom, three-bathroom cabin they finished themselves after Rabjohns, a former nurse, and her husband Ron, a cardiologist, purchased the 35-acre property in 2011. From one of the modest, yet comfortable bedrooms, she explains the choice of locale—close enough to the city for convenience, but far enough to prevent temptation—which is critical to the home’s residents: six recovering addicts and two resident advisors. Open now for two years, Invictus Woods is the only sober living center in Greater Peoria, and that was a large part of the motivation behind building it. But the mission was also personal.
“It hit our family about 13 years ago, and we were stunned,” Camilla explains, outlining her two sons’ recovery from drug and alcohol addictions. “The first time, we didn’t really believe he had an addiction problem, but then it happened to our second [son]… and I thought, ‘I have to educate myself about this.’”
The Rabjohns’ medical background aided their dual mission for the site: to help men recover from addiction, knowing the importance of an extended care program in stabilizing recovery, and to help themselves. “It was important for us personally, and for our own recovery,” Camilla adds.
Physical and Spiritual Recovery
Referrals to Invictus Woods come from area treatment centers; potential residents must successfully complete at least 28 days in a primary-care substance abuse treatment center prior to admission. For the program to be successful, the house must be led by recovered addicts themselves, Camilla explains. Five years clean, her son Nick was ripe for the job.
“The reason they started [Invictus Woods] was because of me and my brother’s struggle with addiction,” Nick admits. “There was nothing like this in the area.” After living in an Oxford House in Maine, he moved back to central Illinois to take on the role of resident supervisor, completing a two-year Drug and Alcohol Counselor Training Certificate at ICC. He and the other resident advisor provide a “long-leashed,” yet structured schedule for the residents. The primary goal, he explains, is to teach them how to function in society again, stressing accountability and responsibility through house chores and division of labor.
“Guys come out here and they get to slow down,” Nick says. A large part of his job, he adds, is simply being there. “If they’re having difficulty and their wheels are turning, and they need to talk to someone… I’m here.” But recovery is an individual process, and it must be self-motivated.
“We follow a 12-step philosophy,” he explains. “I can’t make anybody accept those ideals, and you can’t force a spiritual experience. But if you put them… around other people who have struggled with the same things, the ideas eventually click.”
To prevent relapse, residents are subject to random drug testing, as well as referrals to traditional counselors for additional support during their stay, and they’re driven into town daily as needed. “It’s physical and spiritual recovery,” Rabjohns notes. “Everything helps them get healthier. They come into town; they go to meetings; they work out. They go to the library looking for jobs… We respect them, and we expect them to respect us—to see how normal relationships work, and to get out of relationships that aren’t healthy.”
The Long Road
Taking on her residents’ battles along with those of her sons is a heavy load, Rabjohns admits. “You just become so alone,” she says, “and you start to isolate [yourself].” She has had to find ways to deal with her guilt, and learn how to avoid enabling behaviors.
“Addicts have antennas,” she says. “Their brain just snaps… and that’s all they can think of. They know where to find their drugs, and they know where to find enablers. That’s why it’s so important to go to Al-Anon: so you don’t become an enabler.” She has found peace through the weekly support-group classes.
“You learn how to take care of yourself, and that you only have control over yourself… You think you have control over [your loved ones], but you don’t. You can live by example, and hopefully they’ll learn from that… [but eventually] you have to give control to the higher power.”
One less-discussed element of opioid abuse is its effect on the families of users, and Rabjohns also finds solace in helping them. The Wall Street Journal recently reported that increased abuse of opioids is straining child welfare agencies across the country, at least partially responsible for greater numbers of children in foster care—a 3.5 percent jump in the last year, according to the Administration for Children and Families. This finding highlights the need for increased emotional support for addicts’ families, and Rabjohns makes it a goal to reach out to other mothers of addicts in the area. “I don’t want them to feel alone,” she stresses. “I’m not ashamed of it, and they shouldn’t be. I‘ve learned addiction is a disease; it’s not a disgrace.”
Similarly motivated after losing her 16-year-old son, Joshua, to a heroin overdose in 2012, Dr. Tamara Olt started the JOLT Foundation, a Peoria-based nonprofit that provides overdose prevention services to current and past users, their families and friends. She’s also a prescribing physician of naloxone—the antidote that instantly reverses the effect of an opioid overdose when administered.
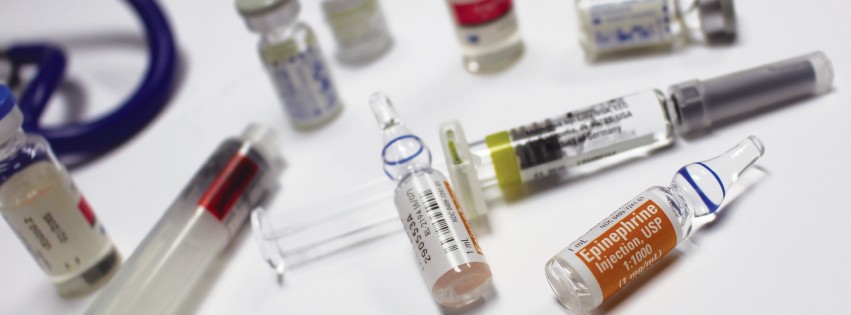
Life-Saving Solutions
Kathie Kane-Willis carries naloxone with her everywhere she goes—the syringes, the drug itself and information, all packaged together in a user-friendly kit. “I remember being on a panel with a bunch of law enforcement officials… talking about the overdose problem and hearing, ‘We don’t know what to do.’ I remember saying, ‘This is what you do,’” she says, recalling pulling out the kit for a demo. “‘You can save people’s lives’… They practically jumped at it.”
A former heroin user herself, Kane-Willis’ past now informs her passion as a researcher, having studied opioid abuse trends for over a decade. In 2004, she began to notice a demographic shift in the data. Users were becoming younger, and were increasingly white, female and living outside of Chicago’s city limits. She and her colleagues at Roosevelt University made recommendations for syringe exchange outreach and additional education on heroin and opioids, well ahead of the curve. “The reception was not warm,” she recalls. “People don’t like it when you say this is happening in their community. So, they push back and deny it… and then you get an HIV cluster,” she suggests—like last year’s tragic outbreak among intravenous drug users in rural Indiana.
In working to heighten public awareness, Kane-Willis has taken countless trips throughout the Midwest, speaking to communities concerned by rising overdose rates. Slowly, through such educational sessions, naloxone has become part of the public sphere, she says. “When people started talking about it, everyone wanted it.”
Also known by the brand name Narcan, naloxone has been approved for use since 1971, but outside of hospitals, few recognized its public health potential early on. The drug’s first take-home program in the U.S. got its start in the 1990s when the Chicago Recovery Alliance launched a “harm-reduction” program in high-risk neighborhoods. Over time, other programs around the country caught on, and the distribution of naloxone continued to increase as the regulations surrounding it eased.
Today, 42 states have laws that address access to naloxone for people at risk of opiate overdose, and 30, including Illinois, provide criminal immunity for prescribers of the antidote. Thirty-three states, also including Illinois, now authorize prescriptions of naloxone by standing order for those at risk, and a few dozen have effectively made naloxone available over the counter.
For Kane-Willis, it’s always been a simple equation. “The amount of naloxone in the community reduces deaths. The more you have, the more deaths are reduced.”
Last fall, all patrol officers with the Peoria Police Department were issued naloxone kits in response to the uptick in overdose cases seen by local emergency responders—about four to eight per week, as reported in October. In some ways, the trend is fundamentally shifting the role of law enforcement officers, who, instead of locking up addicts for possession, now find themselves administering naloxone to save their lives.
Intervention and Understanding
“We’re sort of in this period when people are saying it’s a health crisis, but it’s still a policing issue,” says Kane-Willis, outlining Illinois’ “Good Samaritan” overdose law, passed in 2012, which provides immunity from criminal charges if someone witnesses and seeks medical help for a drug overdose. “The relationship between law enforcement and people who use drugs or who are addicted is an issue that’s always been fraught with a lot of complexity,” she adds.
“Bystander naloxone administration programs have been demonstrated to increase numbers of patients who survive from an opioid overdose. However, they are unlikely to change the prevalence of opioid abuse,” Dr. Yeh explains. Still, he adds, “Expedient administration of naloxone by bystanders may allow time for transport to medical professionals… [and] once stabilized, the patient could then be given resources for substance abuse recovery and overdose education programs.” In addition to saving lives, Kane-Willis agrees, it’s a great opportunity to intervene.
Increased training and greater access to treatment were the goals of the national alarm President Obama sounded in last year’s Presidential Memorandum Addressing Prescription Drug Abuse and Heroin Use. The recommendations call for an acceleration of efforts across the executive branch to increase training of federal healthcare workers in the appropriate prescribing of controlled substances as a model for similar initiatives across the country, and to improve access to medication-assisted treatment in combination with counseling, behavioral therapies and patient monitoring.
Such national efforts are encouraging, suggests Kane-Willis. “We’ve got the federal government really taking the lead,” she notes, but hesitates. “Part of me isincredibly frustrated, because I do think some of [these deaths] could have been prevented if we had implemented some of these solutions [earlier].” A large part of her job at the ICDP involves bridging understanding. “The way most people view the problem is, ‘Let’s just get rid of the heroin,’” she explains. “[But] you can’t! You might think you could do that, but… it doesn’t work. That part requires so much education,” she stresses, as stereotypes run deep. She suggests the societal stigma may not necessarily decrease opioid use, and may even be harmful to those who have become dependent.
 “We forget that these are people,” she says. “Once they become junkies, they… become expendable. But their lives matter. Their lives matter to their families, to their loved ones, to their friends, and to their communities.
“We forget that these are people,” she says. “Once they become junkies, they… become expendable. But their lives matter. Their lives matter to their families, to their loved ones, to their friends, and to their communities.
"We know how to fix this,” she adds. “It’s pretty clear: you need to provide good, medication-assisted treatment, you need overdose prevention programs, you need good Samaritans… and you want to make sure doctors aren’t overprescribing prescription drugs. But we also know if there is a quick cut-down in supply, then you do push people right into the heroin side. So, we need to have bridges. “We need to be talking about drugs and health in more realistic ways, and stop stigmatizing and demonizing it,” she stresses.
“Sometimes the biggest challenge to recovery is finding a provider, making the decision to get the help and for some, having the support to get started,” adds Henry.
But recovery is possible, says Rabjohns. “When you’re diagnosed with addiction, you have it for the rest of your life,” she notes. “Just like diabetes, it doesn’t go away, but you can control it. And people do recover, and they do become successful.” iBi
To learn more about Invictus Woods, visit invictuswoods.com. To obtain a naloxone kit and training in how to administer the antidote, contact the JOLT Foundation at (309) 966-3643, or visit joltfoundation.org.


